Solutions
Healthcare EDI Integration for Every Role
Whether you’re managing EDI operations, making technology decisions, or building integrations — SERENEDI solves the problems you actually face.
For EDI Operations Managers
Stop Firefighting. Start Operating.
You spend your days chasing rejected claims, debugging failed transactions, and explaining to stakeholders why the EDI feed broke again. Your current system gives you error codes but not root causes, and troubleshooting means opening raw X12 files in a text editor.
How SERENEDI Helps
Integrity validation catches errors before they reach your trading partners — checking segment requirements, data types, code sets, and implementation guide rules. When something does fail, the BIZ_MSG audit trail tells you exactly what happened, when, and why.
Business-friendly column names mean you can query your EDI data directly. Find every rejected 837 from last week with a SQL query, not by grepping through flat files. Export to CSV for your analysts or generate HTML integrity reports for your compliance team.
Event-driven automation handles the routine work. Files arrive, get validated, parsed, and loaded — automatically. You manage by exception instead of managing every transaction.
For IT Directors & Architects
Reduce Risk. Control Costs. Ship Faster.
Your EDI integration is either a million-dollar enterprise suite that takes 18 months to deploy, a fragile custom solution that one person understands, or a patchwork of scripts and manual processes that keeps you up at night. None of these options give you what you actually need: reliable, maintainable EDI processing at a predictable cost.
How SERENEDI Helps
Predictable licensing at $4K–$10K/year, no transaction fees. No surprise overages. Snowflake is a flat $5K/year, plus consumer-side utilization costs.
Standard technology stack means your team doesn’t need specialized EDI training. If they know SQL, they can work with SERENEDI.
Two deployment options let you choose the architecture that fits. On-premises with Windows Server and SQL Server for maximum control, or Snowflake Native App for zero-infrastructure cloud deployment. Migrate between them as your strategy evolves.
HIPAA-ready architecture keeps all data within your environment. SERENEDI doesn’t phone home, doesn’t require cloud connectivity (on-prem), and doesn’t store consumer data outside your account (Snowflake). Your compliance team will appreciate the simplicity.
For Developers & Integration Engineers
Build EDI Integrations with Tools You Already Know
You’ve been handed a folder of .edi files and told to “integrate” them with the claims system by next quarter. You open one in a text editor and see a wall of tildes, asterisks, and cryptic codes. The HIPAA implementation guide is 700 pages. The X12 standard is another 1,200. You’re a good developer — but this isn’t code, it’s hieroglyphics.
How SERENEDI Helps
SQL is the interface. Drop an 837 file into a folder. Minutes later, query the claims data with SELECT statements using fields that are rich in business data and minimal metadata.
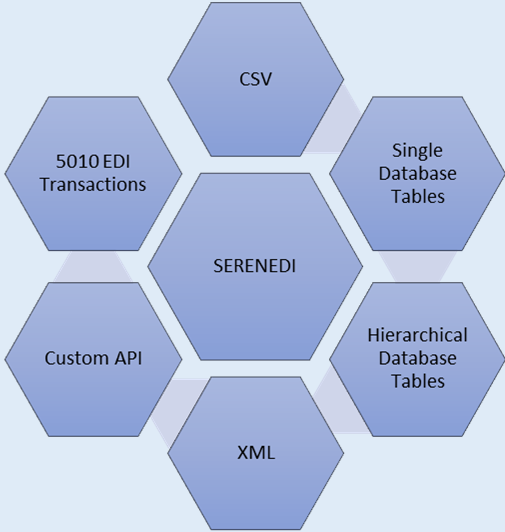
Outbound is just as simple. Populate a CSV or XML file with your data using documented templates, drop it in the outbound folder, and SERENEDI generates a fully compliant X12 transaction. It handles the loops, segments, delimiters – you provide the business data.
Stored procedures give you seed data templates for every supported transaction set. USP_837P_EXTRACT, USP_835_EXTRACT, USP_270_EXTRACT — each one shows you exactly what columns to populate and what values are expected in order to arrive at a valid EDI file.
No proprietary languages or frameworks. Your integration code is standard SQL, PowerShell, or whatever language your team uses. SERENEDI is the translation layer — everything upstream and downstream is in formats you already know.
Common Use Cases
Claims Processing
Parse inbound 837P/I/D claims into SQL tables for adjudication systems. Generate 835 remittances and 277CA acknowledgments from your claims database.
Eligibility Verification
Generate 270 eligibility inquiries from your member data and parse 271 responses back into your system. Automate real-time eligibility checks across your provider network.
Enrollment Management
Process 834 enrollment and disenrollment transactions. Keep your member databases synchronized with payer enrollment feeds automatically.
Remittance Reconciliation
Parse 835 remittance advice into structured tables for payment posting and reconciliation. Match payments to claims, identify adjustments, and feed your revenue cycle.
Prior Authorization
Handle the full 278 workflow — requests, responses, notifications, and acknowledgments. Automate auth submissions and track status through the entire lifecycle.
EDI Analytics & Reporting
Load your EDI data into SQL tables and connect your BI tools directly. Build dashboards, track trends, and generate compliance reports without writing custom parsers.
See How SERENEDI Fits Your Workflow
Schedule a live walkthrough tailored to your specific use case, or download the free evaluation and start exploring with sample data today.
